Description
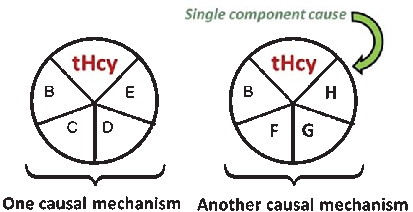
A causal model illustrates how elevated plasma homocysteine may contribute to dementia through multiple pathways, interacting with other risk factors such as age, hypercholesterolemia, and genetic predisposition. No single factor is sufficient alone; rather, combinations of component causes drive disease.
More Figures from This Paper
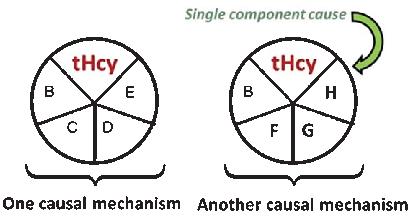
Figure 3
Brain imaging studies demonstrate that elevated homocysteine is associated with accelerated rates of brain atrophy, particularly in medial temporal lobe structures critical for memory. B-vitamin treatment appears to slow this atrophy in individuals with elevated baseline homocysteine.
photograph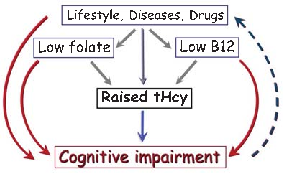
Figure 5
Meta-analyses of cohort studies consistently indicate that elevated homocysteine is associated with approximately doubled risk of Alzheimer's disease. The strength of this association persists after adjustment for common confounders including age, sex, and education.
forest_plotFigure 4
DiagramSource Paper
Homocysteine and Dementia: An International Consensus Statement.Cite This Figure
 > Source: A David Smith et al. "Homocysteine and Dementia: An International Consensus Statement.." *Journal of Alzheimer's disease : JAD*, 2018. PMID: [29480200](https://pubmed.ncbi.nlm.nih.gov/29480200/)
<figure> <img src="https://pdfs.citedhealth.com/figures/29480200/56.png" alt="A causal model illustrates how elevated plasma homocysteine may contribute to dementia through multiple pathways, interacting with other risk factors such as age, hypercholesterolemia, and genetic predisposition. No single factor is sufficient alone; rather, combinations of component causes drive disease." /> <figcaption>Figure 4. A causal model illustrates how elevated plasma homocysteine may contribute to dementia through multiple pathways, interacting with other risk factors such as age, hypercholesterolemia, and genetic predisposition. No single factor is sufficient alone; rather, combinations of component causes drive disease.<br> Source: A David Smith et al. "Homocysteine and Dementia: An International Consensus Statement.." <em>Journal of Alzheimer's disease : JAD</em>, 2018. PMID: <a href="https://pubmed.ncbi.nlm.nih.gov/29480200/">29480200</a></figcaption> </figure>